Sleep Apnea Surgery: An Alternative to CPAP
What is obstructive sleep apnea?
Obstructive sleep apnea is one of the most common sleep-related breathing disorders. Apnea results from the of collapse of the throat tissues and tongue into the airway, causing blockage. The reduced airflow into the blocked airway leads to lowered oxygen levels in the body. The brain then senses the low oxygen and causes a brief awakening to open the airway. This prevents you from getting deep, restful sleep.
What are symptoms of obstructive sleep apnea?
Many people do not remember the brief episodes of awakening during sleep; however, some feel the awakening as a cough or a choking/snorting sensation. Sometimes patients have been told about the presence of loud snoring by friends or family. Other common symptoms include dry mouth upon awakening, frequent nighttime urination and morning headaches. Patients often do not feel refreshed after a night of sleep and experience excessive daytime sleepiness.
What are some of the risk factors for sleep apnea
- Obesity/excessive body weight
- Neck size (circumference) greater than 17 inches (men) or greater than 16 inches (women)
- Older family members with sleep apnea
- Male gender
How do I know if I have sleep apnea?
A physician will initially review your medical history and perform a physical exam. If sleep apnea is suspected, your physician will then have you undergo a sleep study. A sleep study is usually done with you sleeping at home. For some people, the study needs to be done in the hospital. The home sleep study tracks how you breathe providing the doctor with information about breathing effort and oxygen levels. The hospital sleep study monitors your breathing and what happens to your brain and heart during sleep.
The sleep study will diagnose sleep apnea and identify if you have mild, moderate or severe sleep apnea. Your physician will discuss which sleep study is best for you.
What happens if sleep apnea is not treated?
Patients with untreated sleep apnea have an increased risk of developing heart disease, high blood pressure, diabetes and stroke.
What are treatment options for sleep apnea?
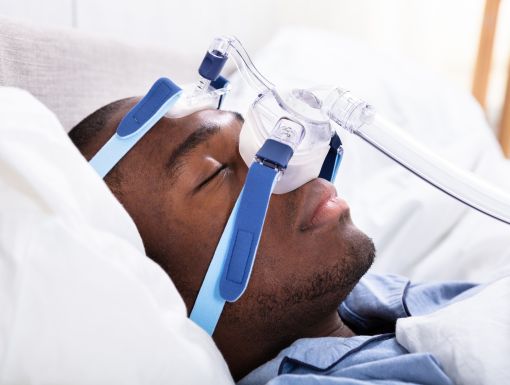
The most common and best treatment for sleep apnea is with continuous positive airway pressure (CPAP). CPAP therapy is a machine that helps patients breathe more easily during sleep. The patient wears a mask over the nose and mouth and the machine delivers air that prevents the throat from collapsing while sleeping. This mechanical airway splint keeps the airway open ensuring the body gets enough oxygen.
Although CPAP is the best treatment, some patients have difficulty with this type of therapy. For these patients, other options may be available. Sometimes in overweight patients with milder forms of sleep apnea, weight loss can treat sleep apnea. Other options include an oral appliance, a device worn in the mouth that helps push the tongue forward. Surgery is also used for treatment in patients that have difficulty using CPAP therapy. One of these surgical options, Inspire, addresses the root cause of sleep apnea by gently stimulating the tongue forward and to keep the throat muscles open while a person is sleeping.
What is Inspire?
Inspire is approved by the U.S Food and Drug Administration for people 18 years or older with moderate to severe sleep apnea. It is the only device to work inside the body using a small implant that sends a pulse to the nerves that signal the tongue to move and open the airway, allowing the patient to breathe freely.
Inspire is implanted inside the body using two small incisions during an outpatient procedure lasting two to four hours. An incision is made in the upper chest to place the device and breathing sensor. The second incision is made under the chin, where a cuff is placed on the nerve that controls the tongue. The cuff communicates with the tongue to move it out of the airway. The battery life for the Inspire device is 11 years. Batteries are replaced with a simple outpatient procedure.
Who qualifies for Inspire?
Ideal candidates for Inspire have been diagnosed with moderate to severe sleep apnea and were unsuccessful in using a CPAP machine. Your doctor will examine your height, weight, body mass index (BMI) and sleep study data. For patients meeting BMI and severity criteria, the next step is an airway evaluation. A tiny camera is used to view how your airway opens and closes during the airway exam while you sleep.
Living with Inspire
After the implant surgery, your physician will teach you how and when to turn on the device. The device is turned on by a small remote held up to the chest. Your physician will work with you to determine the best setting for the device, starting with a low setting and slowly increasing to a higher setting that is comfortable and opens the airway. In research studies, 75% of patients had a cure of sleep apnea and 91% of patients reported satisfaction with inspire due to decreased snoring and reduced daytime sleepiness. The device should be checked once or twice a year by your physician.
***
If you think you are suffering from sleep apnea, consultation with a sleep specialist is recommended. Visit ochsner.org/services/sleep-disorders to schedule an appointment. Learn more about Dr. Jessica Moskovitz.