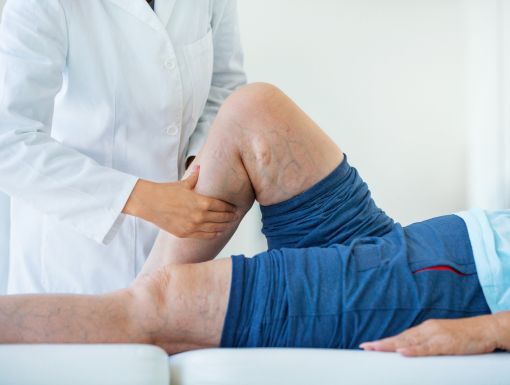
What Causes Varicose Veins?
Are varicose veins dangerous? While most people don’t develop serious problems from varicose veins, it is a common misconception that they are just a cosmetic issue.
When the body is operating as normal, valves in the veins keep the blood flowing towards the heart. When the body is transporting the blood up from the legs, it is working against gravity. If the veins are not working properly, the blood pools in the ankles or legs and pressure begins to build in the veins. This causes the veins to become swollen, weak and lumpy.
According to the American Heart Association, approximately 33 million American adults have varicose veins. Also known as dilated veins, varicose veins result from increased pressure in the leg veins, similar to what causes spider veins. This increased pressure can be due to multiple reasons, such as:
- Weakness in the vein valves (known as venous insufficiency)
- Blood clots
- Compression of the vein
- Lifestyle
What are the symptoms of varicose veins?
Burning, redness and pain are common symptoms associated with varicose veins. A few other signs and symptoms include:
- Bulging veins – swollen, rope-like veins that are often blue or purple in color appear just under the skin. They can develop in clusters and spider veins may appear nearby. This is the most recognizable sign of varicose veins.
- Heavy legs – after physical activity, the muscles in your legs may feel heavy or tired.
- Itching – the area around the veins may itch.
- Pain – legs may become achy, or sores may begin to appear behind your knees.
- Muscle cramps
- Swelling
- Skin discolorations and ulcers – if varicose veins are left untreated, the veins can cause brown discolorations on your skin. If the varicose veins become severe, ulcers may appear on your skin.
Increased pressure in the leg veins can lead to disabling swelling, heaviness, tiredness, and pain, limiting your daily activities. If not treated, worsening pressure can lead to increased leg swelling, wounds and possibly blood clots.
Varicose veins are diagnosed by a physical exam and should be part of your annual physical. Some common risk factors for developing varicose veins include:
- Family history of vein disease
- Female gender
- Age
- Obesity
- Pregnancy
- Tumors
- Prolonged standing or sitting
- Blood clots
- Injury involving the veins
- Smoking
Treatment options for varicose veins
There are many treatment options for varicose veins ranging from devices, lifestyle modifications, medical procedures or surgery. Compression stockings (not socks) can help reduce the pressure in your leg veins, decrease the size of varicose veins and improve symptoms. Prescription compression stockings are designed to apply different amounts of pressure, which helps fluid circulate evenly through.
However, compression stockings are not your only treatment option. Other standard outpatient treatment options include:
- Sclerotherapy: A procedure that involves an injection of a solution into the vein, causing them to collapse, turn into scar tissue and be absorbed by the body.
- Laser therapy also known as endovenous thermal ablation: A minimally invasive procedure in which a laser stops the vein from weakening, reducing the vein's pressure.
- Varicose vein phlebectomy: A minimally invasive procedure that uses a small scalpel or needle to remove veins just below the skin's surface.
Preventing varicose veins may be unavoidable for some people, depending on your family history or other medical conditions. However, there are several things that you can do to reduce the likelihood of varicose veins developing. This includes:
- Daily exercise to improve circulation
- Managing your diet and weight
- Reducing salt intake
- Elevate your legs to help blood flow to your heart
- Avoid standing or sitting for long periods of time
If you are experiencing any symptoms of varicose veins, it’s important to talk to a vascular surgeon about your treatment options. Click here to schedule an appointment with an Ochsner vascular surgeon today.
Ochsner Vascular and Endovascular Surgeons are Nationally Recognized. Make an appointment with our team today.